A root canal is a dental procedure involving the removal of the soft center of the tooth, the pulp. The pulp is made up of nerves, connective tissue, and blood vessels that help the tooth grow.
In the majority of cases, a general dentist or endodontist will perform a root canal while you’re under local anesthesia.
Learn more about this common procedure, as well as the potential risks involved.
When is a root canal needed?
A root canal is performed when the soft inner part of a tooth, known as the pulp, is injured or becomes inflamed or infected.
The crown of the tooth — the part you can see above your gums — can remain intact even if the pulp is dead. Removing injured or infected pulp is the best way to preserve the structure of the tooth.
Common causes of damage to the pulp include:
- deep decay due to an untreated cavity
- multiple dental procedures on the same tooth
- a chip or crack in the tooth
- an injury to the tooth (you might injure a tooth if you get hit in the mouth; the pulp can still be damaged even if the injury doesn’t crack the tooth)
The most common symptoms of damaged pulp include pain in your tooth, and swelling and a sensation of heat in your gums. Your dentist will examine the painful tooth and take X-rays to confirm the diagnosis. Your dentist may refer you to an endodontist if they think you need a root canal.
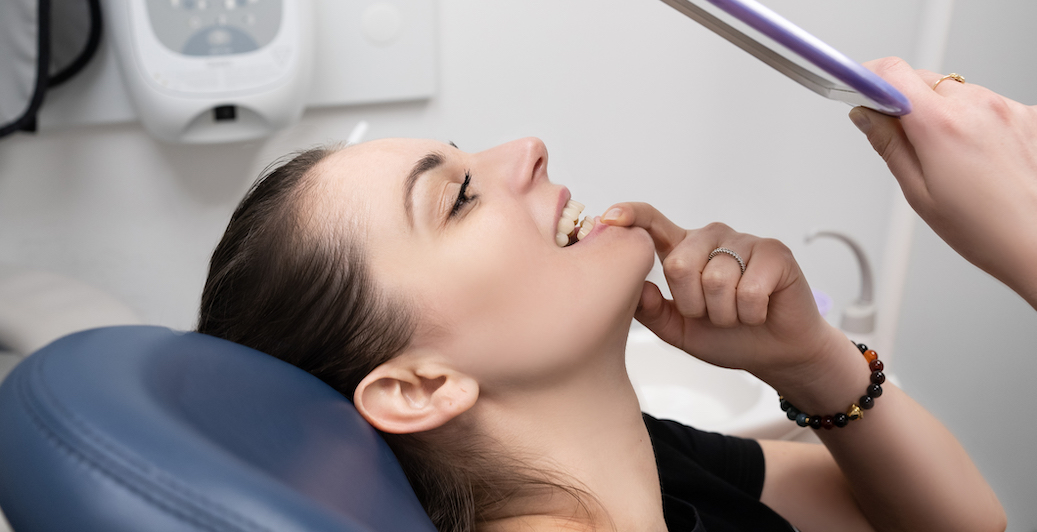
How is a root canal performed?
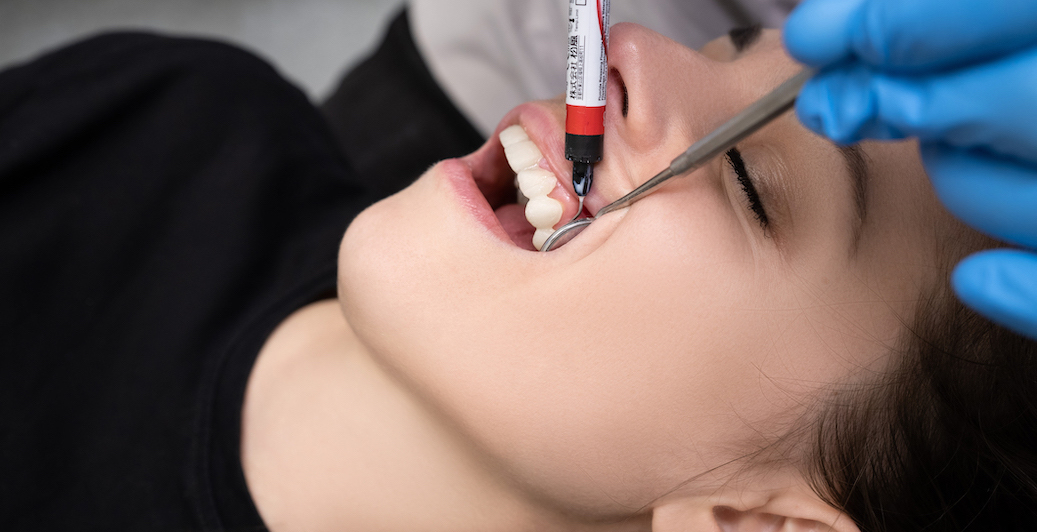
A root canal is performed in a dental office. When you arrive for your appointment, a technician will escort you to a treatment room, help you get situated in a chair, and place a bib around your neck to protect your clothes from stains.
Step 1: Anesthetic
The dentist will place a small amount of numbing medication on your gum near the affected tooth. Once it has taken effect, a local anesthetic will be injected into your gums. You may feel a sharp pinch or a burning sensation, but this will pass quickly.
You’ll remain awake during the procedure, but the anesthetic will keep you from feeling any pain.
Step 2: Removing the pulp
When your tooth is numb, the endodontist or general dentist will make a small opening in the top of the tooth. Once the infected or damaged pulp is exposed, the specialist will carefully remove it using special tools called files. They’ll be particularly careful to clean out all the pathways (canals) in your tooth.
Step 3: Antibiotics
Once the pulp has been removed, the dentist may coat the area with a topical antibiotic to ensure that the infection is gone and to prevent reinfection. Once the canals are cleaned and disinfected, the dentist will fill and seal the tooth with a sealer paste and rubber-like material called gutta-percha. They also may prescribe you oral antibiotics.
Step 4: Temporary filling
The dentist will end the procedure by filling the small opening in the top of the tooth with a soft, temporary material. This sealant helps prevent the canals from being damaged by saliva.
Follow-up after your root canal
Your tooth and gums might feel sore when the numbing medication wears off. Your gums may also swell. Most dentists will have you treat these symptoms with over-the-counter pain medications such as acetaminophen (Tylenol) or ibuprofen (Advil). Call your dentist if the pain becomes extreme or lasts for more than a few days.
You should be able to resume your normal routine the day after the procedure. Avoid chewing with the damaged tooth until it’s permanently filled or a crown is placed over the top.
You’ll see your regular dentist within a few days of the root canal. They’ll take X-rays to make sure that any infection is gone. They’ll also replace the temporary filling with a permanent filling.
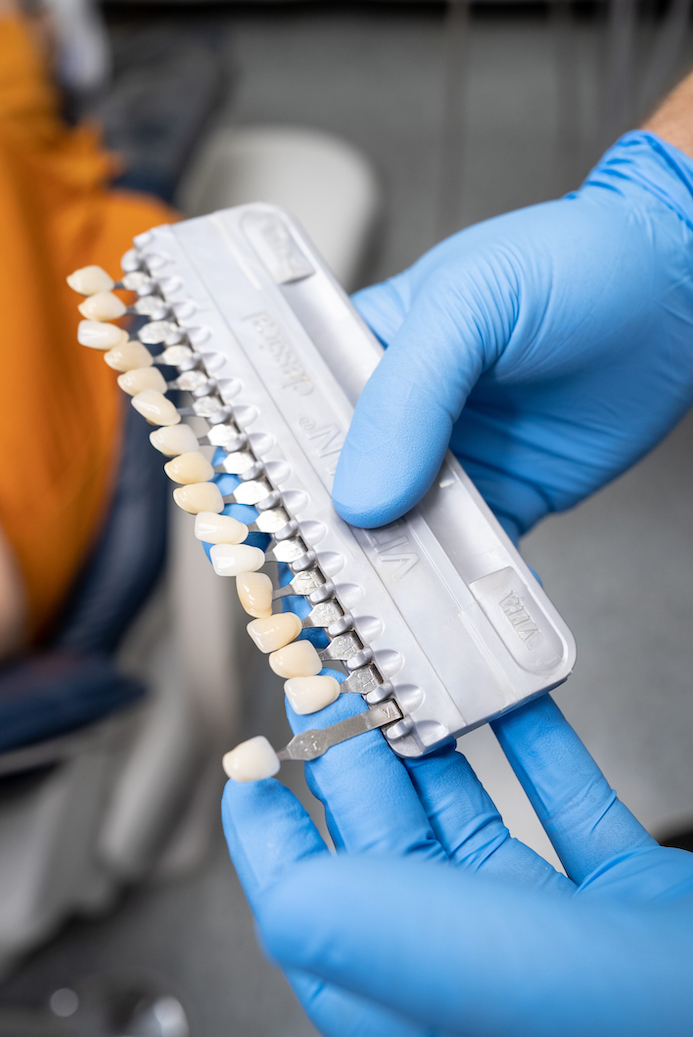
If you prefer, the dentist may place a permanent crown on the tooth. Crowns are artificial teeth that can be made from porcelain or gold. The benefit of a crown is its realistic appearance.
It may take you several weeks to get used to how the tooth feels after the procedure. This is normal and no cause for concern.
Risks of a root canal
A root canal is performed in an effort to save your tooth. Sometimes, however, the damage is too deep or the enamel is too frail to withstand the procedure. These factors can lead to loss of the tooth.
Another risk is developing an abscess at the root of the tooth if some of the infected material remains behind or if the antibiotics aren’t effective.
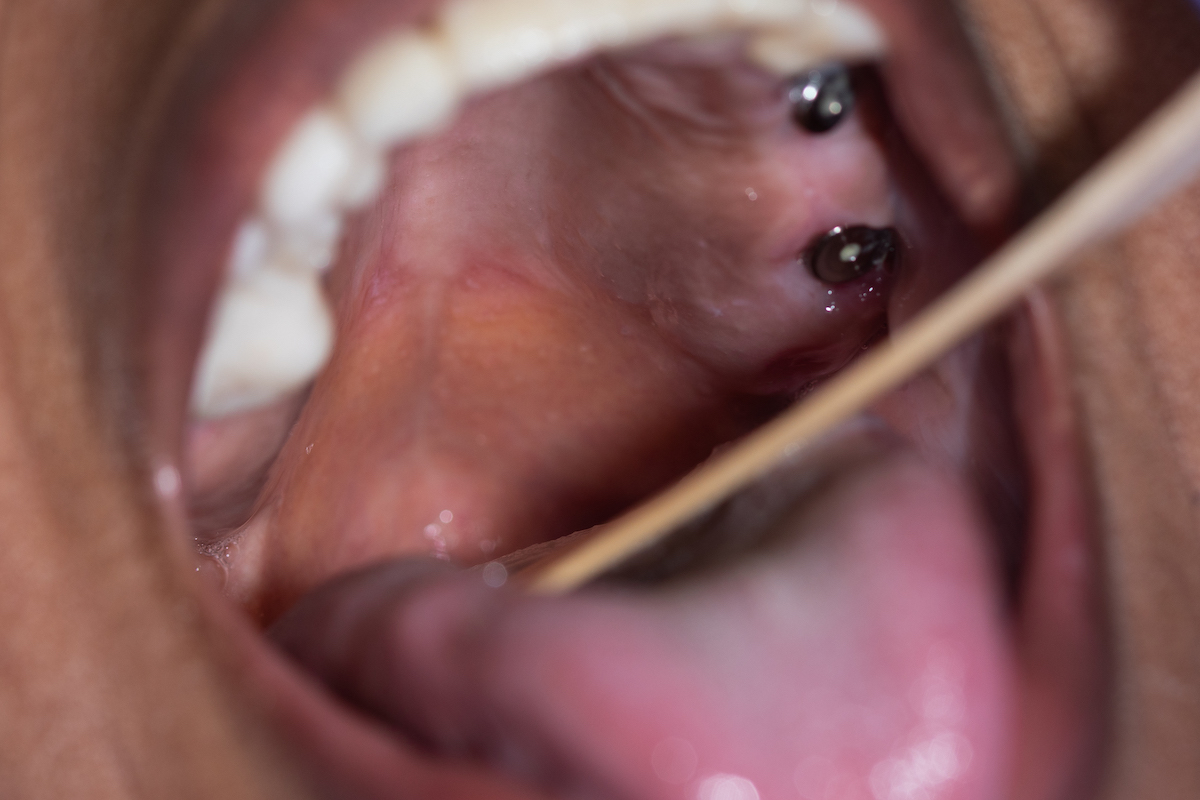
If you’re apprehensive about a root canal, you can talk to your dentist about an extraction instead. This often involves placing a partial denture, bridge, or implant in place of the damaged tooth.
What happens after a root canal?
A root canal is considered a restorative procedure. Most people who undergo the procedure are able to enjoy the positive results for the rest of their lives. Still, how long results last depends on the way you take care of your teeth.
Just as the rest of your teeth depend on good oral hygiene habits, your restored tooth requires regular brushing and flossing as well.